TMD vs TMJ in Tewksbury, MA
Although jaw pain is commonly referred to as “TMJ” even amongst dentists, TMJ stands for TemporoMandibular Joint which is the scientific word for our jaw joint. We all have 2 TMJs, one on each side of our lower jaw. TMDs, or TemporoMandibular Disorders, refer to the group of disorders that cause pain and jaw function problems due to disorders in the bony jaw joint or the muscles and tissue ligaments that support the jaw joints. These jaw muscles can also trigger pain in the muscles of the face and can even cause pain in the associated muscles of the neck as well as migraine headaches on the side and/or back of the head.
Find Relief from Jaw Pain
TMD (Temporomandibular Disorder) and TMJ (Temporomandibular Joint Disorder) can cause chronic pain, discomfort, and even disrupt your everyday activities. If you’re experiencing jaw pain, headaches, or difficulty chewing, TMD could be the culprit. We offer effective, non-invasive treatments to relieve the pain and discomfort caused by TMD and TMJ.
Through advanced therapies like oral appliances, customized mouthguards, and laser treatments, we target the root cause of your jaw issues, offering you long-lasting relief. Our goal is to restore your comfort and help you enjoy a pain-free, active life again.
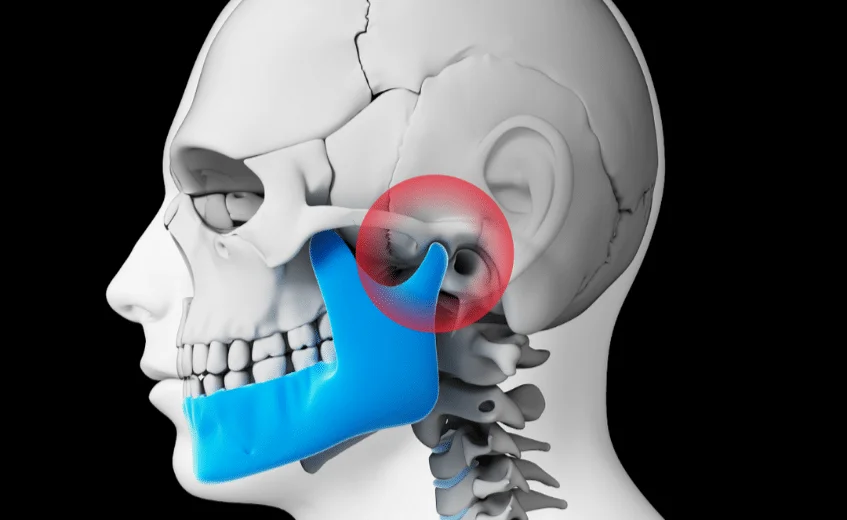

Common symptoms of TMD:
- Jaw and/or tooth pain
- Jaw clicking and/or popping
- Jaw locking or difficulty opening your mouth
- Ear pain, ringing in the ears
- Frequent headaches, jaw pain, neck and/or shoulder pain
- Sensitive teeth, uncomfortable bite
- Grinding and clenching of teeth
- Sleep breathing problems, sleep apnea
What causes TMD and how is it treated?
TMDs are split into 2 broad categories: muscle or tissue related causes vs jaw joint specific causes. The most common cause of TMD, 95% of the time, falls in the muscle and tissue category. This is fortunate because these types of TMD can be well managed with non-surgical treatments. Surgery is not appropriate treatment and should not be recommended for this type of TMD. Since the tissues and muscles surrounding the jaw joint and head area are the cause of the problem, effective treatment is only possible if you identify what is irritating these support structures surrounding the jaw joint. Many times, the problem can be related to someone’s bite or how they hold their jaw during function, at rest and during sleep. Management can include orthopedic mouth appliances, jaw alignment treatments and bite adjustments to get the jaw muscles back into a comfortable position. At times, assessing and managing sleep breathing problems is necessary. Stress and anxiety, systemic body inflammation, and autoimmune diseases can all contribute to TMDs. If your symptoms are truly due to disease in the bony jaw joint from a slipped disk or arthritic changes in the jaw joint, these are the TMD problems that will need to be investigated for possible surgical treatment. These degenerative jaw joint changes could be the result of prior trauma to the face, osteoarthritic disease or chronic jaw joint dislocations that has cause wear and tear disease in the disk and the jaw joint itself.
Who Should I See for Treatment?
Since 95% of all TMDs require non-surgical treatment and are typically related to problems with the bite, the muscles supporting your jaw joint and bite and possible sleep breathing problems, a dental health professional specifically training in evaluating these areas is a good place to start. A detailed history including sleep assessment, and a bite and jaw joint exam with 3D CT imaging is important to help make the right diagnosis. If there are other medical problems that are contributing to your symptoms, a team approach with neurologists, OMTs, upper cervical or atlas-orthogonal practitioners, physical therapists, and others is critical to success and long-term management of symptoms. If the jaw and bite relationship or the airway anatomy is found to be the culprit, custom made orthopedic appliances are typically recommended and made for management along with other non-surgical treatments such as diet changes, hot and cold therapies, jaw exercises, medications and stress management as appropriate. True bony jaw joint disease may also be managed conservatively at times, however if these types of TMDs progress, surgical treatment may become the last option and this would be best performed by a board certified oral and maxillofacial surgeon.
At Solace Wellness Center & MedSpa in Tewksbury, MA, Dr. James Wu has specific training in evaluating and management of these problems. He is a board certified oral and maxillofacial surgeon and can manage surgical problems when needed, however many of these problems can be managed non-surgically by Dr. James Wu as he is a Mentor and Scientific Advisor at the Kois Center in Seattle, WA, a training center Advancing Dentistry through Science.
If you or a loved one suffer from TMD and you’d like to explore your treatment options, reach out to Solace Wellness Center & MedSpa at 978-851-8600 or request an appointment. Our providers will discuss all of the options available to enhance your holistic wellness.
First-time guest?
Enjoy 10% off when you book a series of 3 or more advanced treatments — a perfect way to begin your journey with personalized, results-driven care in a serene, luxurious setting.


